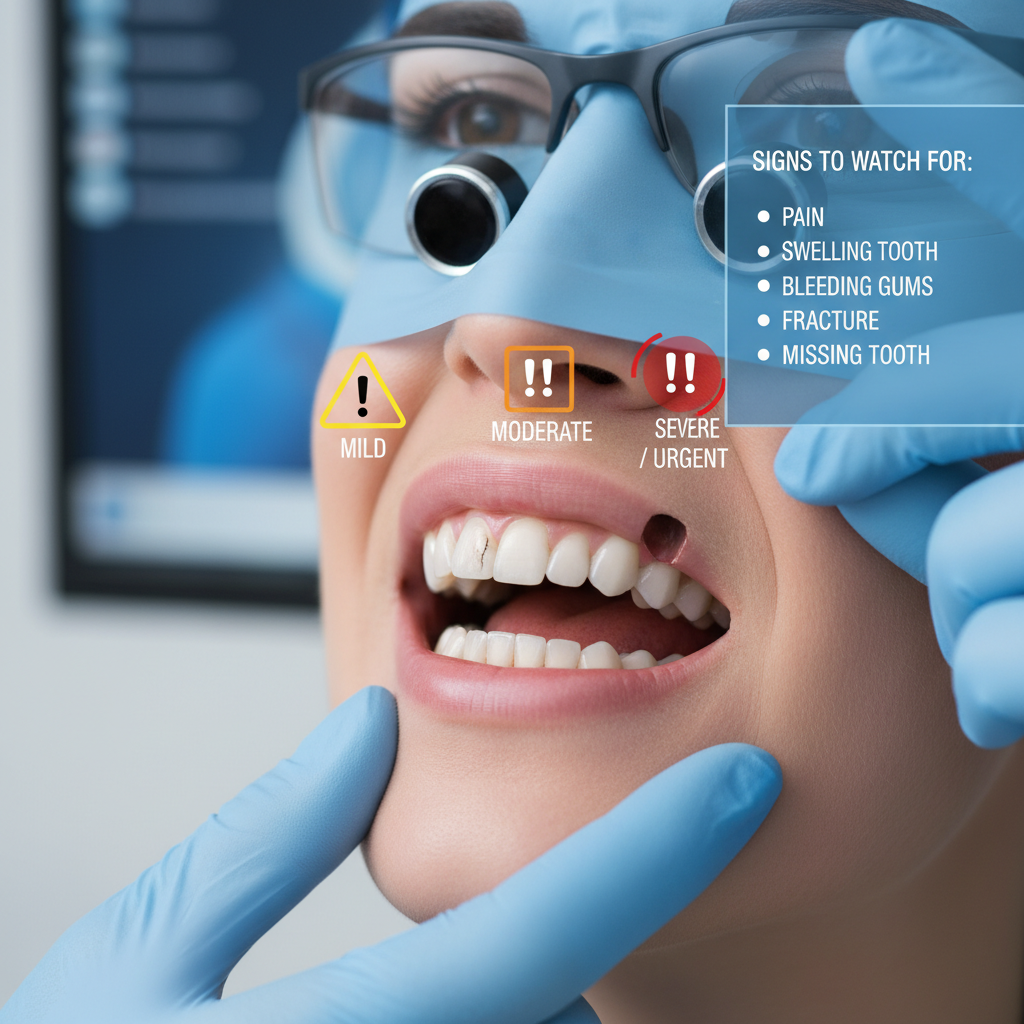
Why dental trauma severity matters
If you injure your teeth or mouth, it can be hard to know how serious the damage really is. Learning how to identify dental trauma severity at home helps you decide when you can safely monitor a problem and when you need immediate care.
Dental trauma covers any injury to your teeth, gums, jawbone, or the soft tissues in your mouth, and it can range from a tiny chip to a completely knocked out tooth or broken jaw [1]. Some situations can wait for a scheduled visit. Others are true emergencies that require fast action to save a tooth or prevent serious complications.
You can use what you see, what you feel, and what happened during the injury to quickly sort injuries into urgent and non urgent problems. This guide walks you through practical steps so you know when to call an emergency dentist and what to do before you get there.
Start with how the injury happened
The way the trauma occurred gives you your first clue about severity. High force usually means higher risk of serious injury, even if the damage is not obvious at first.
Ask yourself:
- Did you fall hard, get hit in the face, or have a sports or car accident?
- Was there enough force to cut the lips or cause bruising or swelling of the face or jaw?
- Were you unconscious at any point, even briefly?
Major impacts, especially with sports equipment, steering wheels, or hard surfaces, are more likely to cause broken roots, jaw fractures, or dislodged teeth. Those injuries need prompt evaluation and often imaging like X rays or CT scans [1].
If the trauma was mild and localized, for example accidentally biting a fork or bumping a tooth lightly, you are more likely to be dealing with a minor chip or soft tissue bruise. These are often less urgent, but you still need to look closely at your teeth and gums.
Check for emergency red flag symptoms
Next, focus on obvious warning signs that require immediate care. These emergency dental warning signs tell you not to wait.
Key red flags include [2]:
- Severe or sudden tooth or jaw pain after a blow to the mouth
- Heavy, continuous, or hard to control bleeding
- A tooth that is very loose, pushed out of position, or completely knocked out
- Obvious facial or jaw deformity, or difficulty opening or closing your mouth
- Trouble moving your jaw or sharp pain when trying to bite or chew
- Swelling or bruising that spreads quickly around the jaw, lips, or cheeks
- Signs of broken facial bones, such as asymmetry, numbness, or a change in your bite
If you notice any of these, you are most likely dealing with a true dental emergency. You should seek immediate care and review resources like what is considered a dental emergency and what dental issues require immediate treatment.
Look closely at your teeth
Once you have checked for obvious red flags, examine each affected tooth in good light. Gently rinse your mouth and use a clean finger or a soft cloth to clear blood or debris so you can see better.
You are looking mainly for:
- Missing teeth or pieces of teeth
- Changes in position or looseness
- Cracks, chips, or breaks
- Color changes of the tooth crown
Knocked out or missing teeth (avulsion)
If a tooth is completely out of the socket, this is called an avulsed tooth. This is one of the most time sensitive dental emergencies.
You can recognize avulsion when:
- The entire tooth is missing from the mouth
- You see an empty socket that may be bleeding
- You have the tooth in your hand, and you can see the crown and root
In this situation:
- Do not touch the root. Handle the tooth only by the crown to protect the delicate cells that help it reattach [3].
- Gently rinse off dirt with milk or saline if available, but do not scrub or use soap [4].
- If possible, gently place the tooth back in the socket and bite on gauze to hold it in place.
- If you cannot reinsert it, keep it moist in milk or in your own saliva. Do not let it dry out.
Avulsed permanent teeth must be treated urgently, ideally within an hour, to maximize the chance they can be saved [4]. This clearly falls in the category of problems that need immediate attention, so reviewing when to go to an emergency dentist is appropriate.
Never try to reimplant a baby tooth. Doing so can damage the developing permanent tooth underneath [3].
Loose, pushed in, or pushed out teeth (luxation and subluxation)
If the tooth is still in the mouth but not in its normal position, you may have a luxation injury. These can range from mild to severe:
- Subluxation: the tooth is slightly loose but still in the correct position
- Extrusion: the tooth is partially out of the socket and looks elongated
- Lateral luxation: the tooth is pushed forward, backward, or sideways
- Intrusion: the tooth is driven deeper into the jaw
You may notice that your bite feels off or it hurts to bring your teeth together. These injuries often need repositioning and splinting by a dentist to heal correctly [4].
Mild loosening with no change in tooth position can sometimes be monitored, but luxation that changes how your teeth fit together or causes significant pain should be considered urgent. For quick guidance in these situations, it helps to review how to tell if you need urgent dental care.
Evaluate chips, cracks, and fractures
Not all broken teeth are emergencies. The severity depends on how deep the damage goes and whether the nerve, or pulp, of the tooth is exposed.
Specialists describe fractures as:
- Uncomplicated fractures: damage to the outer layers of the tooth (enamel and dentin) without exposing the pulp
- Complicated fractures: fractures that expose the pink pulp tissue in the center of the tooth
Uncomplicated fractures often show up as small chips or rough edges. These can usually wait for a regular dental appointment, although you should still be seen soon for smoothing or bonding [3].
Complicated fractures are more serious. You might see:
- A larger chunk of tooth missing
- A visible pink or red spot inside the tooth
- Intense sensitivity or pain to air, cold, or touch
These fractures need prompt treatment to protect the exposed pulp and prevent infection, often within a few days or sooner [3].
If you are unsure whether a chip is serious, exploring topics like is a chipped tooth a dental emergency and is a cracked tooth an emergency can help you decide how quickly to act.
Pay attention to pain and sensitivity
How much something hurts is not the only sign of severity, but it is a key part of your at home evaluation.
Different patterns of pain can suggest different problems:
- Sudden, severe pain right after an injury can point to a crack, nerve involvement, or jaw fracture [5].
- Pain that gets worse when you bite down can indicate a vertical crack or root fracture.
- Throbbing pain that builds over hours or days after trauma may signal developing infection or nerve damage.
Guides like how to know if tooth pain is emergency, how to handle sudden dental pain, and when tooth pain becomes serious can help you connect your symptoms to the level of urgency.
Also be cautious with:
- Pain that wakes you from sleep
- Pain combined with facial swelling
- Pain plus fever or feeling unwell
These can all indicate a spreading infection that requires prompt evaluation, even if your tooth looks mostly normal.
Watch for bleeding and soft tissue injuries
Trauma to the mouth often injures the gums, tongue, inner cheeks, or lips. Sometimes these soft tissue injuries look dramatic but are less serious than damage to the teeth or bone.
You should consider emergency care if:
- Bleeding is heavy or does not slow down after 10 to 15 minutes of firm pressure
- A cut is deep, gaping, or runs through the border of the lip
- There is a flap of tissue that will likely need sutures
- Bleeding seems to be coming from deep around a loose or damaged tooth
Heavy or continuous bleeding around the gums may indicate more serious underlying injury and should be checked quickly [5]. To better understand where bleeding fits on the urgency spectrum, you can review when bleeding gums are an emergency.
Smaller cuts that stop bleeding, along with minor bruising or swelling, can usually be managed at home with gentle rinsing, cool compresses, and monitoring. However, if swelling worsens or you start to have trouble swallowing or breathing, seek emergency medical care right away.
Assess swelling, bruising, and jaw function
Facial swelling and bruising after a blow are common, but certain patterns raise concern about fractures or more severe trauma.
Concerning signs include [5]:
- Rapidly increasing swelling around the jaw, cheeks, or lips
- A noticeable change in your facial shape or symmetry
- Numbness in the lips, chin, or cheeks
- Difficulty opening or closing your mouth
- Sharp pain when moving your jaw
- A bite that suddenly feels off or does not line up normally
These symptoms can suggest a broken jaw or fracture of the bones that support your teeth. Panoramic X rays or CT scans are often used to identify these injuries [3]. If you have this pattern of symptoms, it fits squarely in the category of urgent dental issues and you should not delay care.
If swelling is mild, improves with cold compresses, and your bite feels normal, you are more likely dealing with a moderate injury that can be evaluated on a same day or next day basis rather than in the emergency room. Resources like when gum swelling is an emergency and dental emergency symptoms to watch for can help you monitor your progress.
Understand what you cannot see
One challenge with dental trauma is that serious problems are not always visible at home. Teeth that look normal can still have damaged nerves, hidden cracks, or root fractures.
Studies show that:
- Teeth can develop pulp necrosis, or nerve death, long after the initial trauma, especially if treatment is delayed [6].
- Up to three quarters of teeth that looked normal after trauma later showed signs of nerve death and bone changes on X rays [6].
- Radiographs are essential for detecting root fractures, bone damage, early infections, and resorption that you cannot see with the naked eye [7].
Because of this, even if your at home assessment suggests a minor injury, it is still wise to arrange follow up with a dentist. That visit provides baseline X rays, documentation of the injury, and a plan for monitoring any delayed complications.
If you are trying to decide whether you can wait days or weeks, it helps to look at guidance on how long can you wait for tooth pain and dental emergencies vs routine dental care.
Compare urgent vs non urgent dental trauma
You can think of dental trauma severity on a spectrum from minor problems that can wait to emergencies that require care right away. This simplified comparison may help you decide where your situation fits.
| Situation | Likely urgency | What you should do |
|---|---|---|
| Small chip, no pain, no sharp edges | Non urgent, but should be checked | Schedule a dental visit in the near future. Review urgent vs non urgent dental problems. |
| Moderate chip with sensitivity but no visible pulp | Semi urgent | Call your dentist for a same week appointment. Monitor pain and avoid chewing on that side. |
| Large fracture with pink or red spot visible in the center | Urgent | Seek care within 24 to 48 hours. This is more than a cosmetic issue. |
| Tooth completely knocked out | Emergency | Follow avulsed tooth steps, then go to an emergency dentist or ER immediately. See signs you need emergency dental care. |
| Tooth very loose or moved out of position | Urgent to emergency | Seek same day care, especially if your bite feels off or you cannot close your teeth normally. |
| Heavy, uncontrolled bleeding from mouth | Emergency | Apply pressure and go to an ER or emergency dentist right away. |
| Jaw pain, difficulty opening mouth, facial deformity | Emergency | Go to the ER for imaging and evaluation. |
| Mild swelling and soreness, no loose teeth, normal bite | Semi urgent | Call your dentist for advice, often a same or next day visit is appropriate. |
Resources such as urgent dental issues explained and emergency dental warning signs can further support your decision making.
What to do before you see a dentist
Once you decide that you need care, what you do at home can protect your teeth and reduce complications. Knowing what to do before seeing emergency dentist is especially important after trauma.
General steps include:
- Rinse gently with lukewarm water to clear blood and debris without dislodging clots.
- Apply gentle pressure with clean gauze or a cloth if there is active bleeding.
- Use a cold pack on the outside of the face to limit swelling. Do not put ice directly on teeth.
- Avoid chewing on the injured side.
- If a tooth fragment is available, keep it in milk or saliva and bring it with you. Sometimes it can be bonded back to the tooth [3].
- Take over the counter pain relievers if you can use them safely, but avoid aspirin on open wounds because it can increase bleeding.
If you are not sure whether to go to an urgent care clinic, emergency room, or dental office, reviewing when to go to an emergency dentist and how to tell if you need urgent dental care can help clarify your next step.
When in doubt, contact a dentist
Even with a careful at home assessment, there will be times you are still unsure how serious your dental trauma is. That is normal. The most reliable way to identify dental trauma severity is to contact a dental professional soon after the injury.
Dentists use:
- A focused examination of the teeth, gums, and bite
- X rays and, when needed, CT scans to look for hidden damage [1]
- Established classification systems for traumatic dental injuries to guide treatment decisions [8]
Because time to treatment strongly affects outcomes after trauma, especially for knocked out teeth and injuries in children, it is safer to reach out and be told you can wait than to delay care for a problem that needed immediate attention [6].
If you are debating whether to call, revisit topics like how to know if tooth pain is emergency and what is considered a dental emergency. These can give you extra clarity and confidence as you decide your next step.
By learning how to identify dental trauma severity and combining what you see at home with timely professional advice, you give yourself the best chance to protect your teeth, avoid preventable complications, and get the right level of care at the right time.